
What is ViraFend®?
ViraFend is a natural Virus Attachment Inhibitor and Virus Reproduction Regulator.
ViraFend can support your body’s defense against viruses attaching to human host cells, which is necessary for viruses to reproduce in the body. If a virus cannot attach to a human host cell, it can NOT reproduce.
The Activated Humic Acid in ViraFend works to 'coat' the membrane of virus organisms to inhibit their ability to attach to human cells, and help regulate virus reproduction. If a virus cannot attach to a human cell and insert its genetic material into the human cell, it can not reproduce.
Does ViraFend® cure viruses?
It’s very important to understand that viruses are NOT diseases; they are just organisms. Some viruses can trigger various health issues (such as flu, herpes & cold sore outbreaks, shingles, respiratory viruses and more) when they are allowed to reproduce inside the body unchecked.
The mere presence of a virus is NOT a disease.
ViraFend does not 'cure' or 'prevent' or 'treat' any disease. It works by inhibiting the ability of viruses to attach to human host cells, and thus regulates virus reproduction.
How do we know ViraFend® works?
The active ingredient in ViraFend – Humic Acid – has been extensively tested by the National Institutes of Health and it was shown to be effective against every virus it was tested against, and has been studied for more than 50 years in numerous peer-reviewed scientific studies.
Can I take ViraFend® if I already have a virus?
YES! ViraFend has been clinically shown to be an effective 'virus attachment inhibitor' and a 'virus reproduction regulator'. If you have NOT been exposed to a virus, and have ViraFend in your system, the active ingredient in ViraFend will 'coat' the virus and interfere with its ability to attach to a human cell. If you have already been exposed to, or infected by a virus, when the virus reproduces in the body, ViraFend's humic acid will inhibit the ability of the newly reproduced viruses to spread to new host cells once it has started to reproduce.

ViraFend Inhibits Virus Attachment to Human Cells to Help Regulate Virus Reproduction
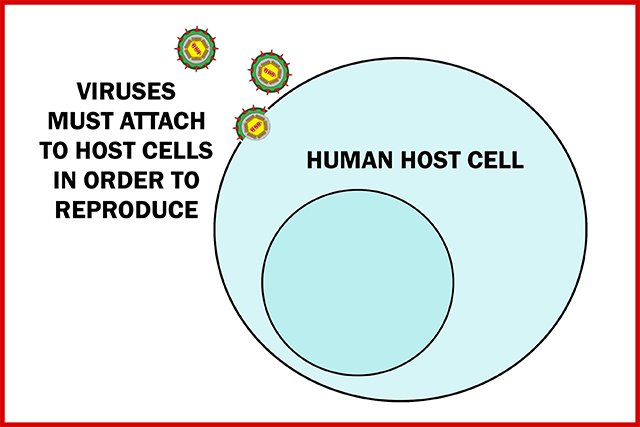
Viruses cannot reproduce by themselves. In order to reproduce, a virus must first attach itself to a human host cell, and hijack that cell's reproductive mechanisms to replicate.
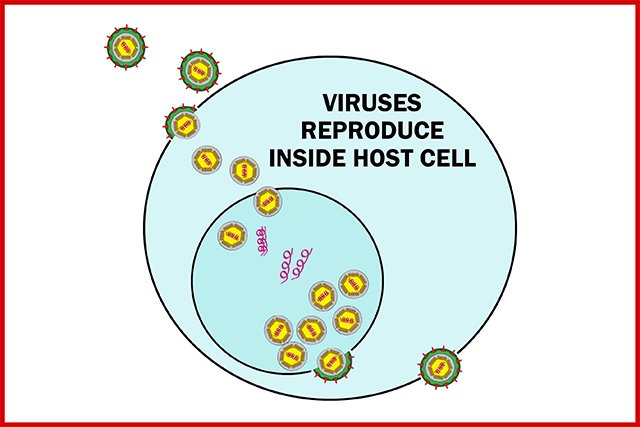
Viruses use human host cells as incubators to reproduce millions of new virus particles. Each new virus particle produced exits the host cell to find a new host cell to attach to, and the cycle repeats over and over.
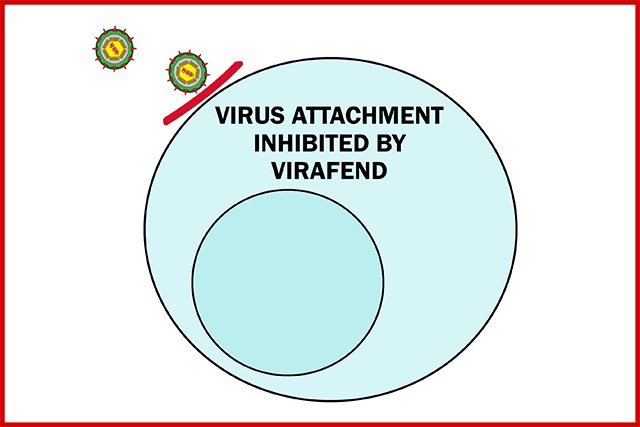
If a virus organism can't attach to a human host cell, the virus life cycle can't proceed, and the virus is inhibited from reproducing. This is known as 'Virus Attachment Inhibition".
Each bottle (60 capsules) is a full 1-month's supply.
Scientific studies have shown that the active ingredient in ViraFend – activated humic acid – effectively inhibits the ability of multiple viruses to attach to human cells. In order to reproduce, a virus must attach to a human host cell and reproduce inside those cells. If a virus cannot attach to a host cell, it cannot reproduce. In extensive clinical studies and scientific research over 50 years, the active ingredient in ViraFend has been shown to safely and effectively inhibit virus attachment to human host cells and help regulate virus reproduction.

Activated Humic Acid - The primary active ingredient in ViraFend® Virus Defense Formula - has been tested by the NIH and found effective against every virus tested.
The official scientific measure of a substance’s potency against a virus or biological agent is called the EC50 test – which measures the level of the substance being tested to achieve a 50% 'effectiveness' against the virus the substance is being tested against.
EC50 levels are scored, with a LOWER EC50 meaning a greater potency and effect against the virus.
Following is a summary table of the EC50 levels validated by the National Institutes of Health, Virology Branch in Bethesda, MD.
| Virus Designation | Virus Common Name | EC50 Levels | Effectiveness Rating |
|---|---|---|---|
| Infl A – H1N1 | NSW Flu Virus | 1.3 | ✔ Effective |
| Infl A – H1N1 | Puerto Rico Flu Virus | 18 | ✔ Effective |
| Infl A – H3N2 | Shangdong Flu Virus | 18 | ✔ Effective |
| Infl A – H3N2 | Sydney Flu Virus | 0.35 | ✔ Effective |
| Infl B | Harbin Flu Variant | 0.7 | ✔ Effective |
| Infl B | Hong Kong Flu Virus | 3.2 | ✔ Effective |
| HSV-1 | Oral Herpes Virus | 4.7 | ✔ Effective |
| HSV-2 | Genital Herpes Virus | 2.5 | ✔ Effective |
| HCMV | Cytomegalovirus | 32.3 | ✔ Effective |
| MCMV | Cytomegalovirus M | 33.3 | ✔ Effective |
| VZV | Varicella/Zoster (Shingles) | 53.5 | ✔ Effective |
| EBV | Epstein-Barr Virus | 50 | ✔ Effective |

*These statements have not been evaluated by the Food & Drug Administration. These products are not intended to diagnose, treat, cure or prevent any disease. Always seek professional medical attention for any medical conditions or health issues you may be experiencing. The information on this website is not intended as medical advice or to replace the advice of a qualified medical professional.